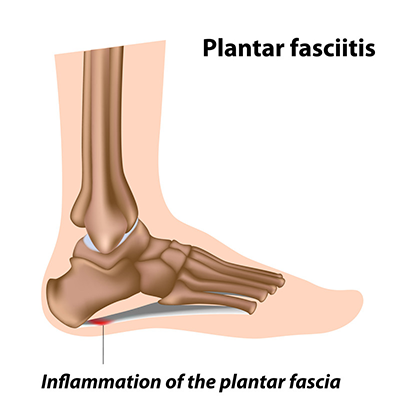
Plantar fasciitis (also known as plantar fasciopathy or jogger’s heel) is a common painful disorder affecting the heel and underside of the foot. It can progress to bony heel spur if the problem is longstanding and at the origin of the fascia. The plantar fascia is a thick fibrous band of connective tissue that originates from the medial tubercle and anterior aspect of the calcaneus (shown below). The fascia extends along the sole of the foot before inserting at the base of the toes, and supports the arch of the foot.
Plantar fasciitis got part of it’s name, ‘itis’, as it was believed to be an inflammatory condition. However, studies have observed microscopic anatomical changes indicating that plantar fasciitis is actually due to a non-inflammatory structural breakdown of the plantar fascia rather than an inflammatory process (Tahririan et al., 2014 and Yin et al., 2014). Due to this shift in thought about the underlying mechanisms in plantar fasciitis, many in the academic community have stated the condition should be renamed plantar fasciosis. The breakdown of the plantar fascia is still believed to be the result of repetitive microtrauma (Monto, 2013 and Orchard, 2012). Microscopic examination of the plantar fascia often shows myxomatous degeneration, connective tissue calcium deposits and disorganized collagen fibres (Lareaur et al., 2014)
Standing and walking mechanically incorrectly (known as the Windlass mechanism) are thought to place excess strain on the calcaneal tuberosity leading to the problem (Yin et al., 2014). Other studies have also suggested that plantar fasciitis is not actually due to inflamed plantar fascia, but may be a tendon injury involving the flexor digitorum brevis muscle located immediately deep to the plantar fascia (Orchard 2012).
Shockwave therapy for plantar fasciitis has been extensively studied with a reported success rate from 34% to 88% (Buch et al, 2002, Chen, Chen & Huang, 2001, Chuckpaiwong, Berkson & Theodore, 2009, Gerdesmeyer et al, 2008, Gollwitzer et al, 2007, Hammer et al, 2003, Hyer, Vancourt & Block, 2005, Ibrahim et al, 2010, Kudo et al, 2006, Metzner, Dohnalek & Aigner, 2010, Norris, Eickmeier & Werber, 2005, Ogden et al, 2004, Rajkumar & Schmitgen, 2002, Rompe et al, 2003, Rompe, Schoellner & Nafe, 2002, Wabg et al, 2000, Wang, Chen & Huang, 2002, Wang et al, 2006, Weil et al, 2002).
The majority of the published papers report a positive and beneficial effect. Rompe, Schoellner & Nafe (2002) have shown that shockwave is an effective therapy for plantar fasciitis with significant alleviation of pain and improvement in function. Wang, Chen & Huang (2002) showed at one year follow-up the overall results were 75.3% complaint free, 18.8% significantly better, 5.9% slightly better and none unchanged or worse. The recurrence rate was 5%. They concluded that shockwave therapy is a safe and effective modality in the treatment of proximal plantar fasciitis.
In contrast, few studies reported the opposite results of ESWT in the treatment of plantar fasciitis (Buchbinder et al, 2006, Buchbinder et al, 2002, Speed et al, 2003, Greve et al, 2009, Haake et al, 2003).
Buchbinder et al (2002) said there was no evidence to support a beneficial effect of shockwave over placebo (on pain, function and quality of life). Haake et al (2003) compared shockwave to placebo. Their results showed that shockwave was ineffective in the treatment of chronic plantar fasciitis. In a randomised double blind control trial, Speed et al (2003) found no treatment effect of moderate dose shockwave in subjects with plantar fasciitis. Efficacy may be highly dependent upon machine types and treatment protocol (Speed et al, 2003). Therefore, controversy exists on the effect of ESWT in the treatment of chronic plantar fasciitis. Wang (2012) said the differences are probably due to the methodology, patient selection criteria, use of different devices, different energy levels/total energy and the outcome measurements.
Several studies have compared the effects of shockwave with surgery, local corticosteroid injection or physical (physio) therapy in the treatment of proximal plantar fasciitis (Weil et al, 2002, Othman & Ragab, 2010, Yucel et al, 2010). Comparison of surgical treatment (plantar fasciotomy) and shockwave showed comparable functional outcomes (Weil et al, 2002). Physical (physio) therapy has shown to be comparable to or even better than shockwave in proximal plantar fasciitis, however, no one has yet studied them in combination (Greve, Grecco & Santos-Silva, 2009). Corticosteroid injection shows better short-term effects, but the long-term results favour shockwave (Yucel et al, 2010).
The application of ESWT in proximal plantar fasciitis is performed with either local anaesthesia or no anaesthesia. Several reports showed that ESWT is less effective when the treatment is performed with the use of local anaesthesia (Labek et al, 2005, Rompe et al, 2005).
Wang (2012) said in summary, the literature review reveals discrepancy and controversy on the effect of shockwave on plantar fasciitis. Many factors can influence the effects of shockwave in the treatment of plantar fasciitis. The vast majority of the published papers are in favour of ESWT. Additional studies are needed to validate the effectiveness of ESWT in the treatment of plantar fasciitis.
Treatment parameters depend on whether the treatment is for a particular spot or the whole of the fascia (some people do the whole fascia after a spot anyway).
Single Spot:
Settings: Anywhere from 1.8 bar or 80-90mj up to 4.0 bar or 150mj. Normally 8-12hz (lower is more painful) for 2000 shocks.
Frequency: Repeated every 5 to 7 days. Sessions as required to eliminate the pain (normally 3-6 but can be a lot more).
Whole structure:
Settings: From 1.8 bar or 80-90mj up to 2.8 bar or 120mj. Normally 12-15hz for 2000 shocks moving the head.
Frequency: Repeated every 5 to 7 days. Sessions as required to eliminate the pain (normally 3-6 but can be a lot more).